Weight Loss Surgery – Shape Your Body, Shape Your Tomorrow
Introduction
Weight loss surgery, medically known as weight reduction or metabolic surgery, is one of the most effective treatments available today for people struggling with severe obesity. Unlike short-term solutions such as fad diets, supplements, or temporary exercise programs, weight loss surgery is designed to deliver long-lasting results by making permanent changes to the digestive system.
Globally, obesity has become a serious health challenge. Millions of people live with obesity-related conditions such as type 2 diabetes, high blood pressure, cardiovascular disease, fatty liver disease, and joint problems. While some individuals succeed with non-surgical approaches like diet modification and structured physical activity, many others fail to maintain weight loss in the long run. For such patients, weight loss surgery provides a powerful, proven solution.
This guide explains everything you need to know about weight loss surgery—what it is, how it works, who it is for, different types of procedures, recovery process, risks, benefits, lifestyle changes, and long-term results. By the end, you will have a clear and thorough understanding of this life-changing medical intervention.
What is Weight Loss Surgery?
Weight loss surgery refers to a group of surgical procedures that help individuals lose weight by changing the way the stomach and digestive system handle food. These surgeries primarily work in two ways:
- Restriction: Making the stomach smaller so that patients feel full with less food.
- Malabsorption: Bypassing parts of the small intestine so the body absorbs fewer calories and nutrients.
Many procedures combine both effects, offering maximum weight reduction and metabolic improvements.
Additionally, weight loss surgeries affect hormones related to appetite and metabolism. For example, by reducing the production of the hunger hormone ghrelin, these surgeries decrease food cravings and promote healthier eating habits.
It is important to understand that weight loss surgery is not a quick fix. It is a tool that works best when patients commit to long-term lifestyle changes such as balanced nutrition, regular exercise, and ongoing medical follow-up.
Why Weight Loss Surgery is Performed
Doctors recommend weight loss surgery for individuals who are severely obese and have not been able to lose weight through traditional methods like diet, exercise, or medication. The primary reasons for undergoing the surgery include:
- Health Improvement: Obesity significantly increases the risk of life-threatening conditions such as diabetes, high blood pressure, heart disease, stroke, kidney disease, and certain types of cancer. Surgery helps reduce these risks.
- Enhanced Quality of Life: Patients often experience better mobility, reduced joint pain, improved sleep, and more energy for daily activities.
- Psychological Well-being: Many people struggling with obesity face depression, anxiety, and social stigma. Weight loss improves self-esteem and emotional health.
Who is Eligible for Weight Loss Surgery?
Doctors use specific medical criteria to decide if someone qualifies for weight loss surgery. Typically, candidates include:
- Adults with BMI ≥ 40 (extreme obesity).
- Adults with BMI between 35 and 39.9 who also have obesity-related health problems such as type 2 diabetes, sleep apnea, or heart disease.
- Adolescents with a BMI ≥ 40, or BMI ≥ 35 with severe health complications.
Before approving surgery, patients undergo:
- A complete physical and metabolic evaluation.
- Nutritional and psychological assessments.
- Pre-surgery lifestyle changes such as quitting smoking, limiting alcohol, and starting light exercise.
Medical Conditions Treated by Weight Loss Surgery
Weight loss surgery can significantly improve or even resolve multiple obesity-related diseases:
- Type 2 Diabetes: Improves insulin sensitivity and often leads to long-term remission.
- High Blood Pressure: Weight reduction eases cardiovascular strain.
- High Cholesterol: Helps normalize lipid levels, lowering the risk of heart attack or stroke.
- Heart Disease: Enhances heart function and reduces artery plaque.
- Sleep Apnea: Eliminates or reduces breathing difficulties during sleep.
- Fatty Liver Disease: Reduces fat buildup and inflammation in the liver.
- Joint Pain & Osteoarthritis: Less weight reduces stress on joints.
- Kidney Disease: Slows obesity-related kidney damage.
- Cancer Risk: Lowers the likelihood of obesity-related cancers.
Common Myths About Weight Loss Surgery
- Myth: Surgery is an “easy way out.”
Fact: It requires lifelong commitment to diet, exercise, and medical follow-up. - Myth: Only the extremely obese should consider surgery.
Fact: Patients with moderate obesity and serious health risks may also benefit. - Myth: Surgery is unsafe.
Fact: Modern minimally invasive (laparoscopic) techniques make it as safe as many common operations like gallbladder removal. - Myth: Weight regain is guaranteed.
Fact: With discipline and follow-up care, long-term weight maintenance is highly achievable.
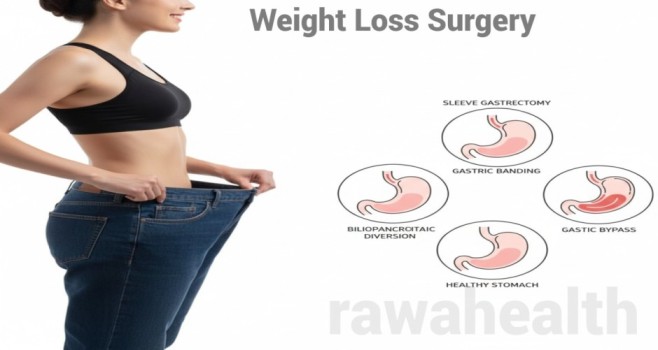
Types of Weight Loss Surgery
There are several surgical options. Each has unique benefits, risks, and suitability depending on the patient’s health and goals.
1. Gastric Sleeve (Sleeve Gastrectomy)
- Around 75–80% of the stomach is removed.
- Leaves a narrow tube or “sleeve.”
- Patients feel full quickly and eat less.
- Reduces hunger hormones (ghrelin).
- Average weight loss: 30–80% of excess body weight.
- Simpler than bypass, with lower complication risk.
2. Gastric Bypass (Roux-en-Y)
- Creates a small stomach pouch.
- Bypasses part of the small intestine.
- Combination of restriction + malabsorption.
- Highly effective for long-term weight loss.
- Average weight loss: 60–70% of excess body weight.
- Especially effective for patients with diabetes.
3. Adjustable Gastric Band
- A band is placed around the upper stomach.
- Creates a small pouch that fills quickly.
- Less invasive, but weight loss is slower.
- Requires frequent adjustments.
- Less common today but still an option.
4. Biliopancreatic Diversion with Duodenal Switch (BPD-DS)
- Removes a large part of the stomach.
- Bypasses nearly 75% of the intestine.
- Very effective for severe obesity and diabetes.
- High risk of nutritional deficiencies.
- Requires strict lifelong vitamin and mineral supplements.
5. Stomach Intestinal Pylorus-Sparing Surgery (SIPS / SADI-S)
- A newer variation of duodenal switch.
- Uses a single intestinal bypass connection.
- Reduces complication risks while maintaining effectiveness.
- Long-term results are still being studied.
Weight Loss Surgery Cost in India
| City | Cost Range (USD) |
|---|---|
| Delhi | $3,000 – $5,000 |
| Mumbai | $3,800 – $7,500 |
| Chennai | $3,200 – $6,500 |
| Bangalore | $3,400 – $6,700 |
| Hyderabad | $3,000 – $6,000 |
| Jaipur | $3,500 – $6,000 |
Cost Comparison: India vs. Other Countries
| Country | Cost Range (USD) |
|---|---|
| India | $3,500 – $6,000 |
| United States | $17,000 – $26,000 |
| United Kingdom | $10,900 – $20,500 |
Pre-Surgery Preparation
Patients preparing for surgery go through several important steps:
- Medical Testing: Blood work, imaging, and heart/lung evaluations.
- Nutritional Counseling: Education about dietary changes.
- Mental Health Check: Assess readiness for lifestyle changes.
- Lifestyle Adjustments: Stopping smoking, reducing alcohol, and beginning light activity.
This preparation reduces risks and ensures smoother recovery.
Surgical Procedure
- Most surgeries are performed laparoscopically (small incisions, camera-guided instruments).
- Minimizes scarring, reduces pain, and speeds up recovery.
- Surgery usually takes 2–4 hours.
- Hospital stay: 2–5 days.
- Patients are closely monitored in recovery for complications.
Post-Surgery Recovery
Hospital Phase
- Vital signs monitored continuously.
- Pain management with medications.
- IV fluids until liquids are tolerated.
Home Recovery
- Light walking encouraged to improve circulation.
- Gradual diet transition:
- Liquids
- Pureed foods
- Soft foods
- Regular balanced meals
- Supplements required: multivitamins, calcium, vitamin D, B12, and iron.
- Most patients return to normal activities within 2–4 weeks.
Long-Term Lifestyle Changes
- Dietary Habits
- Smaller, protein-rich meals.
- Avoid sugary, fried, and processed foods.
- Stay hydrated (but limit fluids with meals).
- Exercise
- Aerobic exercise (walking, cycling, swimming).
- Strength training for muscle retention.
- Flexibility and balance training.
- Psychological Support
- Counseling and support groups.
- Mindful eating practices.
- Stress management and emotional care.
Expected Weight Loss & Health Benefits
- Sleeve Gastrectomy: 30–80% of excess weight loss.
- Gastric Bypass: 60–70% of excess weight loss.
- Duodenal Switch: Up to 80% of excess weight loss.
Health improvements include:
- Diabetes remission or control.
- Reduced cholesterol and blood pressure.
- Relief from sleep apnea.
- Better mobility and less joint pain.
- Longer life expectancy (40% reduction in mortality risk).
Risks and Complications
Like any major surgery, weight loss surgery carries risks:
- Surgical Risks: Bleeding, infection, blood clots, leaks, or hernias.
- Digestive Issues: Dumping syndrome, reflux, gallstones.
- Nutritional Deficiencies: Vitamin and mineral shortages.
- Weight Regain: Possible if lifestyle changes are ignored.
With regular follow-ups and supplements, most risks can be prevented or managed.
Long-Term Success Strategies
- Commit to balanced diet + regular exercise.
- Take prescribed vitamins and minerals daily.
- Stay connected with your healthcare team.
- Attend support groups for motivation.
- Monitor weight regularly and make timely adjustments.
Conclusion
Weight loss surgery is a powerful medical tool for individuals struggling with obesity and related health conditions. It offers sustainable results when combined with a healthy lifestyle and ongoing medical follow-up. Patients not only achieve weight loss but also experience dramatic improvements in overall health, longevity, and quality of life.
For anyone considering this option, the journey requires commitment, discipline, and continuous support, but the rewards—both physical and emotional—are truly life-changing.
Our Step-by-Step Process – How We Work
- Initial Consultation: Understand medical history, concerns, and goals for personalized guidance.
- Personalized Treatment Plan: Customized plan with recommended treatment, costs, and timeline.
- Travel & Preparation: Visa, airport transfers, accommodation, and language support.
- Scheduling & Procedure: Treatment at top hospitals with experienced doctors using advanced technology.
- Aftercare & Follow-Up: Nursing care, follow-ups, and continuous support for smooth recovery.
Why Patients Choose India for Medical Treatment
- Expert Doctors & Specialists: Highly skilled, internationally trained doctors handle advanced procedures and complex surgeries.
- State-of-the-Art Hospitals: Modern hospitals with latest technology and international accreditations ensure world-class treatment.
- Affordable Costs: Medical care in India is 30%–70% cheaper than in Western countries without compromising quality.
- Quick Access: Minimal waiting times allow patients to get treated promptly.
- End-to-End Support: Visa, airport transfers, accommodation, language translation, and post-treatment follow-up provided.
- High Success Rates: Proven track record in surgeries, transplants, and advanced treatments.
- Personalized Care: Individual attention ensures a smooth, safe, and comfortable medical journey.
Get Started with Rawa Health Services
- If you’re considering treatment in India, Rawa Health Services will guide you every step of the way:
- ✅ Free Pre-Surgery Consultation
✅ Doctor & Hospital Appointment
✅ Visa & Travel Assistance
✅ Airport Pickup & Accommodation
✅ Post-Treatment Support
✅ Multilingual Translators for Your Native Language - 📞 Call/WhatsApp: +91-9990978550
📧 Email: rawahealthservices@gmail.com