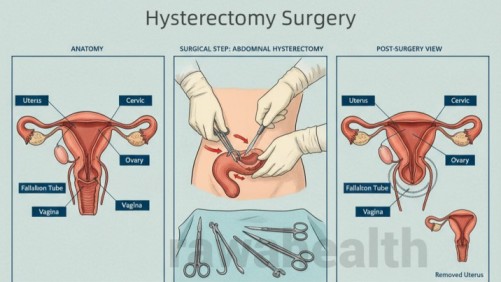
Hysterectomy Surgery – Safe Procedure, Recovery & Costs - Overview
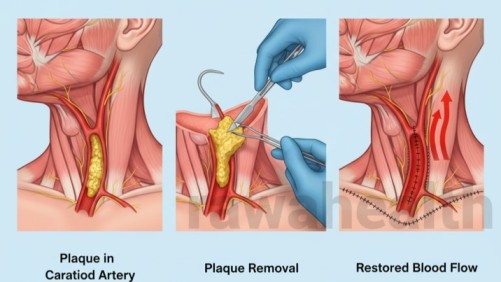
Hysterectomy is a surgical operation in which the uterus is removed, sometimes along with other reproductive organs. After this procedure, a person can no longer become pregnant and menstruation stops permanently. It is usually considered when other treatments fail or when a serious medical condition makes surgery the best option. Recovery typically requires four to six weeks, although the exact time depends on the type of surgery and the individual’s overall health.
What is a hysterectomy?
In its most basic form, a hysterectomy removes the uterus, and in many cases, the cervix as well. Depending on the underlying health issue, the surgeon may also remove the ovaries, fallopian tubes, and surrounding tissues. Once the uterus is removed, the ability to conceive ends, and menstrual periods do not return.
Different types of hysterectomy
There are several variations of hysterectomy, each tailored to the patient’s condition:
- Total hysterectomy – The uterus and cervix are removed, while the ovaries remain in place. Because the ovaries are intact, menopause does not occur immediately after surgery.
- Supracervical hysterectomy – Only the upper part of the uterus is removed, leaving the cervix behind. The fallopian tubes and ovaries may or may not be removed at the same time. Regular Pap tests are still needed because the cervix remains.
- Total hysterectomy with bilateral salpingo-oophorectomy – This involves removing the uterus, cervix, both fallopian tubes, and ovaries. Once the ovaries are gone, menopause begins right away if it has not already occurred naturally.
- Radical hysterectomy with bilateral salpingo-oophorectomy – In addition to the uterus, cervix, fallopian tubes, and ovaries, this procedure removes the upper portion of the vagina, surrounding tissues, and often lymph nodes. It is most often performed when cancer is present. Menopause begins immediately if the ovaries are removed.
Conditions treated with hysterectomy
Doctors usually try alternative treatments before recommending hysterectomy, but in some cases surgery is the only effective solution. Common reasons for undergoing this procedure include:
- Abnormal or heavy vaginal bleeding
- Chronic pelvic pain that does not respond to other treatments
- Uterine fibroids or other noncancerous tumors
- Severe endometriosis
- Uterine prolapse, which may cause urinary or bowel problems
- Cancers of the cervix, uterus, or ovaries
- Conditions affecting the uterine lining, such as adenomyosis or hyperplasia
- Life-threatening complications from childbirth, including uterine rupture
Some individuals choose hysterectomy as a preventive measure, particularly those at high risk of developing cancer in the reproductive organs. Removing the uterus and other reproductive structures significantly reduces the risk of certain cancers.
Procedure Details
Preparing for a hysterectomy
Before surgery, patients typically meet with their healthcare provider to discuss the type of hysterectomy recommended, possible risks, and expected recovery. Blood and urine tests are usually ordered to confirm that the patient is healthy enough for surgery. In some cases, imaging tests may also be performed to help the surgeon plan the procedure.
Depending on the type of hysterectomy and the surgical approach, a hospital stay may or may not be required. Vaginal and laparoscopic procedures are often outpatient surgeries, while abdominal hysterectomy usually involves a few days of hospitalization. Patients are encouraged to arrange support at home for the first few weeks after surgery.
What happens during surgery?
On the day of surgery, the patient changes into a hospital gown and is connected to monitors for heart rate, oxygen levels, and blood pressure. An intravenous (IV) line is inserted into the arm to provide fluids and medications.
An anesthesiologist administers either:
- General anesthesia – inducing complete unconsciousness for the duration of the surgery.
- Regional anesthesia (epidural or spinal) – numbing the lower half of the body while the patient remains awake, though this is less common for hysterectomy.
The surgical team then proceeds using one of several different methods, chosen based on the patient’s diagnosis, medical history, and overall health.
Surgical approaches to hysterectomy
Vaginal hysterectomy
- The uterus is removed through an incision at the top of the vagina.
- No abdominal incisions are made, and dissolvable stitches close the surgical site internally.
- This approach typically has the fewest complications and the fastest recovery (two to four weeks).
- Many patients return home the same day.
Vaginal laparoscopic hysterectomy
- A laparoscope (a thin tube with a camera) is inserted into the pelvic area to provide a clearer view.
- The uterus is removed through the vagina, without abdominal cuts.
- Recovery is generally shorter and less painful than abdominal laparoscopic methods.
- Many patients are discharged on the same day.
Abdominal laparoscopic hysterectomy
- A small incision is made near the navel to insert the laparoscope.
- Additional small incisions are made for surgical instruments.
- The uterus is removed in small sections through these incisions or through the vagina.
- Hospital stays are usually short, ranging from same-day discharge to an overnight stay.
Robotic-assisted laparoscopic hysterectomy
- Similar to standard laparoscopy, but robotic technology assists the surgeon with greater precision.
- Several small incisions are made for instruments, which the surgeon controls remotely.
- Recovery is comparable to laparoscopic hysterectomy, with less pain and quicker return to normal activity compared to open surgery.
Abdominal hysterectomy
- A larger incision (6–8 inches) is made in the lower abdomen, either vertically or horizontally across the pubic area.
- The uterus is removed through this incision, which is closed with stitches or staples.
- This method is often used when cancer is suspected, the uterus is enlarged, or disease has spread beyond the uterus.
- It usually requires a two- to three-day hospital stay and a longer recovery time of four to six weeks.
How long does surgery take?
The average hysterectomy lasts one to three hours. Duration depends on the size of the uterus, whether scar tissue is present from past surgeries, and if additional structures such as ovaries or endometriosis tissue must also be removed.
Pain and side effects
Anesthesia ensures patients feel no pain during the operation. Afterward, it is common to experience soreness, fatigue, and mild discomfort for a few weeks. Pain management may include prescription medications or over-the-counter options like NSAIDs or acetaminophen.
Short-term side effects may include:
- Light vaginal bleeding or discharge
- Incision site soreness
- Difficulty passing urine or stool in the initial days
- Fatigue due to the body’s healing process
If ovaries are removed during hysterectomy, menopausal symptoms can appear immediately. These include hot flashes, vaginal dryness, sleep disturbances, and reduced libido. Hormone replacement therapy may be suggested to manage these symptoms.
Managing menopausal symptoms after hysterectomy
When ovaries are removed during a hysterectomy, the body abruptly enters menopause. This sudden change can feel overwhelming, as hormone levels drop quickly rather than gradually. Common symptoms include:
- Hot flashes and night sweats
- Vaginal dryness leading to discomfort during intercourse
- Sleep problems and mood swings
- Thinning of bones (osteoporosis) over time
Doctors often recommend hormone replacement therapy (HRT) to ease these symptoms, unless contraindicated by other health issues such as certain cancers. Non-hormonal strategies—like regular exercise, a calcium-rich diet, and stress reduction practices—also play an important role in long-term health.
Recovery and Aftercare
Immediate recovery in hospital
After surgery, patients are taken to a recovery room where vital signs are monitored closely. Most individuals stay in the hospital for several hours (for minimally invasive surgery) or up to three days (for abdominal hysterectomy). Nurses encourage walking as soon as possible, since light movement reduces the risk of blood clots.
Pain is managed through medication, and an IV may remain in place for fluids and antibiotics. A urinary catheter is often used during the first day to make urination easier.
At-home recovery timeline
Week 1–2
- Rest is essential, but short walks around the house are encouraged.
- Heavy lifting, bending, or straining should be avoided.
- Vaginal bleeding may continue lightly, but should gradually lessen.
Week 3–4
- Energy levels begin to improve, though fatigue may persist.
- Patients can usually resume light household activities.
- Driving may be allowed if no longer taking strong pain medication.
Week 5–6
- Most women feel stronger and can return to work, depending on the job.
- Exercise routines can slowly resume under medical guidance.
- Sexual activity can usually be restarted after medical clearance.
Long-term recovery and adjustments
- If the ovaries were removed, menopausal symptoms may last for several years.
- Weight gain can occur due to hormonal changes and reduced activity. A balanced diet and regular physical activity are important for managing weight.
- Emotional adjustments are also common. Some women experience relief, while others struggle with feelings of loss related to fertility. Support groups and counseling can be very helpful.
Risks and Complications
While hysterectomy is generally safe, as with all surgeries, there are potential risks:
- Surgical risks: bleeding, infection, injury to nearby organs (bladder, ureters, or intestines)
- Blood clots: deep vein thrombosis (DVT) or pulmonary embolism (PE)
- Anesthetic complications: reactions to medication or breathing problems
- Long-term effects: pelvic organ prolapse, changes in bladder or bowel function, early onset of menopause
Prompt medical attention is needed if patients experience:
- Severe pain not relieved by medication
- High fever or chills
- Heavy vaginal bleeding with large clots
- Difficulty urinating or bowel obstruction
- Swelling, redness, or pain in the legs (possible clot)
Life After Hysterectomy
Most women report significant improvement in symptoms such as pain or heavy bleeding. Energy often improves once recovery is complete. Maintaining bone health, heart health, and hormonal balance becomes a long-term focus, especially if the ovaries were removed.
Sexual health
Many women are able to enjoy a fulfilling sex life after hysterectomy. In fact, relief from pain or bleeding can improve intimacy. However, vaginal dryness or changes in sensation may occur. Using lubricants, vaginal estrogen creams, or undergoing pelvic floor therapy can be beneficial.
Mental and emotional wellbeing
The emotional impact varies greatly. Some women feel empowered and relieved, while others grieve the loss of fertility or feel anxious about body changes. Open conversations with healthcare providers, therapists, and loved ones can help with these adjustments.
Alternatives to Hysterectomy
Hysterectomy is often seen as a last resort. Depending on the condition, less invasive treatments may be available:
- Medication – hormonal therapy (birth control pills, IUDs, or injections) can reduce heavy bleeding or regulate cycles.
- Endometrial ablation – destroys the uterine lining to reduce bleeding, but pregnancy afterward is unsafe.
- Myomectomy – removes fibroids while preserving the uterus.
- Uterine artery embolization (UAE) – shrinks fibroids by blocking blood supply.
- Physical therapy – can help manage pelvic pain caused by non-cancerous conditions.
Doctors usually evaluate the severity of symptoms, the desire for future pregnancy, and the patient’s age before recommending hysterectomy.
Cost of Hysterectomy in India vs Abroad
The cost of hysterectomy varies widely depending on the country, hospital, surgical approach, and whether insurance is available.
- India: The average cost ranges from $3,000 to $5,000 (USD) depending on the city, type of hospital, and surgical method. Minimally invasive techniques (laparoscopic/robotic) may cost slightly more than vaginal or abdominal methods. However, India remains one of the most affordable destinations for hysterectomy while offering world-class healthcare facilities and experienced surgeons.
| Country/Region | Average Cost (USD) |
|---|---|
| India | $3,000 – $5,000 |
| United States | $15,000 – $25,000 |
| United Kingdom | £7,000 – £12,000 |
| Middle East / Europe | $8,000 – $18,000 |
Success Rates
Hysterectomy is considered one of the most successful gynecological surgeries in terms of symptom relief and patient satisfaction.
- Symptom relief: More than 90% of women experience significant improvement in heavy bleeding, pelvic pain, or fibroid-related symptoms.
- Surgical safety: Mortality rates are extremely low (less than 1 in 1,000 cases) when performed by skilled surgeons.
- Complications: Serious complications are rare and occur in less than 5% of cases. These may include infection, bleeding, or injury to nearby organs.
- Quality of life: Studies show that the majority of patients report improved physical and emotional well-being within months after recovery.
Final Thoughts
Hysterectomy is a major decision, but for many women it brings long-term relief from severe symptoms and improves quality of life. With advanced surgical methods available in India and abroad, patients now have safer, faster, and more effective options than ever before.
A clear understanding of costs, recovery, risks, and benefits helps women make informed choices. Consultation with a qualified gynecologist is essential to determine whether hysterectomy—or an alternative treatment—is the best path forward.
Our Step-by-Step Process – How We Work
- Initial Consultation: Understand medical history, concerns, and goals for personalized guidance.
- Personalized Treatment Plan: Customized plan with recommended treatment, costs, and timeline.
- Travel & Preparation: Visa, airport transfers, accommodation, and language support.
- Scheduling & Procedure: Treatment at top hospitals with experienced doctors using advanced technology.
- Aftercare & Follow-Up: Nursing care, follow-ups, and continuous support for smooth recovery.
Why Patients Choose India for Medical Treatment
- Expert Doctors & Specialists: Highly skilled, internationally trained doctors handle advanced procedures and complex surgeries.
- State-of-the-Art Hospitals: Modern hospitals with latest technology and international accreditations ensure world-class treatment.
- Affordable Costs: Medical care in India is 30%–70% cheaper than in Western countries without compromising quality.
- Quick Access: Minimal waiting times allow patients to get treated promptly.
- End-to-End Support: Visa, airport transfers, accommodation, language translation, and post-treatment follow-up provided.
- High Success Rates: Proven track record in surgeries, transplants, and advanced treatments.
- Personalized Care: Individual attention ensures a smooth, safe, and comfortable medical journey.
Get Started with Rawa Health Services
- If you’re considering treatment in India, Rawa Health Services will guide you every step of the way:
- ✅ Free Pre-Surgery Consultation
✅ Doctor & Hospital Appointment
✅ Visa & Travel Assistance
✅ Airport Pickup & Accommodation
✅ Post-Treatment Support
✅ Multilingual Translators for Your Native Language - 📞 Call/WhatsApp: +91-9990978550
📧 Email: rawahealthservices@gmail.com